Lees je liever de Nederlandse versie?
This article is part of “The Polyvagal World” on RelaxMore.net and is intended as an accessible starting point for anyone who is new to polyvagal theory. Additional articles on RelaxMore.net and in the Relaxicon explore specific themes such as neuroception, co-regulation, and fawning in greater depth. Questions are welcome in the comments.
Introduction
Polyvagal theory is about the communication between the brain and the body. It describes how internal and external signals—largely outside our conscious awareness—influence our sense of safety and guide our behavior. The theory offers insight into the intelligence of our evolutionary heritage: over millions of years, that heritage has shaped our nervous system with one purpose in mind: to protect us and enable us to function optimally within our environment.
The theory touches on several disciplines at once: psychology, physiology, evolutionary biology, and neurology. This synthesis sometimes complicates it, but also especially valuable—it connects what mainstream medicine still too often treats in isolation.
Are you a therapist or healthcare provider interested in this material?
I have developed a two-day training program (in Dutch): “Polyvagal Theory and Trauma Responses” — in-depth theory with practical application.
The Science of the Feeling of Connection and Safety
“The great thing then, in all education,
is to make our nervous system our ally,
as opposed to our enemy.”
William James, 1914
It is remarkable that William James already sensed in 1914 how decisive our nervous system is for our well-being. Exactly eighty years later, Stephen Porges gave this scientific grounding in polyvagal theory. Safety—or rather, the inner experience of safety—plays a central role:
“How safe we feel is crucial to our mental and physical health and happiness.”
Stephen Porges
What Is Polyvagal Theory About?
The autonomic nervous system—the part that unconsciously regulates all kinds of bodily functions—turns out to be more than just a control system for our physiology. It also contains the core structures that allow us to experience safety or threat. Polyvagal theory describes what one might call the language of our autonomic nervous system.
Professor of psychiatry and neuroscientist Stephen Porges published the theory in 1994. He shows how the evolution of our autonomic nervous system explains why we respond to stress, threat, and social contact the way we do. In doing so, he draws connections between autonomic dysregulation and a broad range of physical and mental complaints.
Polyvagal theory is increasingly concerned with connection and love: with the factors that make connection possible, and with what happens when that connection is absent. In this way, it also offers guidance for broader social questions: how do we make the world a safer place?
Polyvagal theory is about how our body responds to the various challenges of life. These responses are rooted in the evolution of our autonomic nervous system. Throughout our evolutionary history as vertebrates, that autonomic nervous system has gradually changed. In the process, new pathways or circuits have emerged. These circuits function in a hierarchy; the newer circuits inhibit the older ones. Those older circuits are the defense or protection circuits. In medicine and various therapies, we are now gaining greater insight into the role that a dysregulated autonomic nervous system plays in many diseases, especially chronic ones. The autonomic nervous system also exerts a significant influence on mental health.
A poorly regulated autonomic nervous system—in other words, one that is dysregulated, or out of balance—may, according to polyvagal theory (PVT), help explain several gastrointestinal complaints (including constipation, irritable bowel syndrome, and spastic colon), most post-traumatic symptoms, sensory hypersensitivity, and some features associated with autistic traits.
What is particularly valuable about Porges’ work is that he not only developed a theory but also foresaw its practical implications. He proposes alternative, more body-oriented treatment options, which have already produced good results. Recently, Porges has devoted increasing attention in his work to the practical implications of polyvagal theory.
Polyvagal theory is increasingly about love and connection. The theory sheds light on the factors that make connection possible, but also on the factors that play a role when we miss or lose connection. Through this new science, we can learn what in our society will help make the world a more loving place.
What Does ‘Polyvagal’ Mean?
Poly means ‘multiple’; vagal refers to the vagus nerve, one of the most important cranial nerves in our body. Polyvagal therefore, means ‘multiple vagal pathways.’ The impression may arise that the theory is only about the vagus nerve, but that is not the case. Four other cranial nerves also play a role, and the theory describes the entire autonomic nervous system as an integrated whole.
How Does Polyvagal Theory Stand Scientifically?
Polyvagal theory has found broad acceptance in clinical practice—in trauma care, body-oriented therapy, and developmental psychology. Pioneers such as Peter Levine (Somatic Experiencing®), Bessel van der Kolk, and Pat Ogden recognized in Porges’ work the neurobiological explanation they had been searching for—the one that confirmed what they had been observing in the treatment room for years: the path to trauma healing runs through the body.
At the same time, there is scientific debate. The most prominent criticism comes from researchers Grossman and Taylor, who raised questions about a number of anatomical and evolutionary details of the theory—particularly regarding the interpretation of the vagus nerve and the evolutionary ordering of vagal circuits. Porges has responded to this criticism and refined parts of his formulation. That debate is not fully closed, and rightly so: this is how science works.
The core of polyvagal theory—that our autonomic nervous system operates within a hierarchy of survival circuits and that safety is the foundation for connection and recovery—stands firm as a clinical explanatory model and continues to be substantiated. Elsewhere on this website I discuss the scientific debate in greater depth; the website of the Polyvagal Institute (and here the Dutch foundation) is also worth following in this context.
“Knowledge is meaningless until it lives in the body.”
Peter Levine
The Three Pillars of Polyvagal Theory
Polyvagal theory rests on three interconnected insights. In most accounts, these pillars are listed in the same order: (1) Autonomic Hierarchy, (2) Neuroception, and (3) Co-regulation.
The first pillar receives the most attention in the literature, but that is not, in my view, a reason to describe it first in this overview. I now prefer a ‘chronological sequence’: what happens, step by step, in real life? That gives a different order:
Neuroception (the scanning process that sets everything in motion), and then, on the basis of that scanning, the regulation of the…
Autonomic hierarchy.
Co-regulation comes third, though it remains a somewhat tricky concept wherever you place it.
Ordinarily, a paywall would appear here — but because I consider this an important article for anyone with an interest in polyvagal theory, I have removed the paywall for this article.
Pillar 1: Neuroception — Our Unconscious Safety Radar
Our nervous system continuously scans the environment, our body, and the relational field for signals of safety or threat. This happens at lightning speed, automatically, and entirely outside our conscious awareness. Porges calls this process neuroception: the neural detection of safety, danger, or life threat.
Neuroception differs from perception. Perception is conscious awareness; neuroception is a deeper, older system that responds before the cerebral cortex has processed the information. This explains why we sometimes feel tense in a situation that ‘objectively’ seems safe or why we relax while others remain worried: our neuroception is responding to subtle signals we do not consciously notice.
The Three Information Channels of Neuroception
Neuroception draws on three streams of information to determine whether the current place and moment are safe or whether there is danger or life threat:
External signals: environmental sounds, light intensity, spatial openness or enclosure, the familiarity of a place, and all other information coming in through the senses.
Internal signals: muscle tension, heart rate, breathing, gut feelings, pain, fatigue, nausea, temperature sensation, hunger, thirst—in short, everything that arrives via interoception (the ‘inner senses’).
In people with a chronic condition, this channel is especially relevant and often especially problematic: the body continuously sends signals of unsafety or threat—pain, exhaustion, discomfort—causing neuroception to be structurally colored toward danger, even when no external threat is present. This explains why chronic pain and fatigue are so closely intertwined with autonomic dysregulation.
Relational signals: these are signals that come directly from the nervous system of another person—tone and quality of voice, facial expression and eye contact, body posture and movement, and the quality of touch. It is not the environment or context as such, but what the other body radiates and what our nervous system picks up from it, before we do anything consciously with it.
Based on this scanning process—which takes place around the clock, using ancient brain structures in the brainstem and surrounding subcortical areas to analyze the incoming information from all three streams — the nervous system determines which autonomic state (Pillar 2) is appropriate, and automatically ‘switches’ to it. We do not choose this; our body does it for us.
Where our consciousness enters the picture is when we notice that our autonomic state has changed—for example, that our heart rate has gone up or that we feel more or less tense.
When Neuroception Makes ‘Mistakes’
We are all generally born with a reasonably well-calibrated neuroception. Our neuroception is ‘trained’ by the experiences we go through and can become dysregulated in the process. In people with a trauma history, neuroception may detect danger where none exists, or miss genuine threat signals. A relatively neutral remark from a colleague is experienced as an attack; a crowded room triggers panic; intimate contact feels unsafe. This is not a conscious choice or ‘overreacting’; it is a nervous system that has learned to be extra vigilant.
In people who experienced severe stress very early in life—for example, a premature birth, medical interventions as a newborn, or even significant stress in the womb — neuroception may be calibrated toward threat from very early on. In my articles on GHIA, I write more about this.
These insights have major consequences for how we relate to people who react strongly to situations that seem neutral to us. The question should not be ‘Why is he or she making such a fuss?’ but rather ‘What is this person’s nervous system detecting that mine is not?’ or perhaps even better, ‘What have you been through?’
Our neuroception does not make mistakes; it has been calibrated based on our experiences. Its intention has always been, and still is, to help us survive in a way that costs as little energy as possible.
Pillar 2: The Evolutionarily Shaped Autonomic Hierarchy
Now that we understand how the nervous system scans the environment (neuroception) — and how this forms the basis for regulating autonomic state—let us look at what the available options actually are.
Polyvagal theory describes that we humans share the same survival strategies as other mammals. When we feel safe, we are more inclined to seek connection with one another. This happens via the so-called ventral vagal circuits. One might also call this the ‘connection system’. In this state, we are able to feel compassion, comfort others, and behave in a friendly and understanding way. We feel more caringly connected to ourselves, and we are able to learn.
When neuroception detects a threat, a number of responses become available. These are often presented as a predictable, stepwise sequence of responses. Reality is somewhat less linear, but for now we will use the standard sequence.
First, we try to resolve a threatening situation by establishing a social connection. We ask for help or offer to help. The connection system is further activated. If this does not lead to a restoration of safety and connectedness, we then automatically engage our sympathetic nervous system (the action system) to flee from or fight against the source of threat. Fight and flight sometimes occur literally, but today more often figuratively—for example, raising one’s voice or blaming others (fight) or changing the subject or acting very busy (flight).
If activating the action system does not produce the desired effect, we ultimately fall back on the dorsal vagal circuits (let us call this the rest-and-withdrawal system), which immobilizes us in a freeze response. In this state, we feel helpless, powerless, and shut down.
Polyvagal theory thus describes three levels for dealing with stress and threat: three hierarchically organized subsystems of the autonomic nervous system.
The confusion often lies in the word hierarchical. The hierarchy is not so much about which state is activated after which; rather, it refers to evolutionary age and the fact that ‘newer’ systems inhibit the ‘older’ ones. In evolutionary terms, the rest-and-withdrawal system is the oldest, followed by the action system, with the connection system being the most recent.
We use our higher, newer brain structures to inhibit our older defense systems when there is no danger. An evolutionarily determined hierarchy—or, in more formal language, a phylogenetic ordering (i.e., the developmental history of a species).
Summary
For clarity, the following sequence is useful:
In safety, or when safety is in question: seeking contact and social connection via the connection system. If that is not sufficient…
When there is danger or apparent danger, switching to mobilization—the action system activates via the fight-and-flight response. If that also fails…
Then there is apparently a life threat: a response of immobilization or freezing arises via the rest-and-withdrawal system.
This sequence suggests too rigid an order; for sensitive readers, a value judgment may also seem implicit—as if having the connection system activated is somehow better than having one of the other two active. The sequence fits with the concept of an autonomic ladder, an image widely used to explain polyvagal theory and one that has been very helpful but for which we now have better alternatives.
As we already concluded in the section on neuroception, the goal of the whole process is to ensure our survival. There are therefore no ‘wrong’ autonomic states; they are all adaptive—a response to the situation as neuroception has interpreted it.
Not Only in the Face of Threat
These systems do not only activate in response to stress and threat; they are also active in daily life. Our autonomic nervous system is always ‘on,’ 24 hours a day. Even when we experience no threat, the three systems are active in some combination. When exercising, the action system is active—but without threat being present; when meditating, the rest-and-withdrawal system comes to the foreground—again, without threat. This is an important addition that polyvagal theory has contributed.
Mixed States
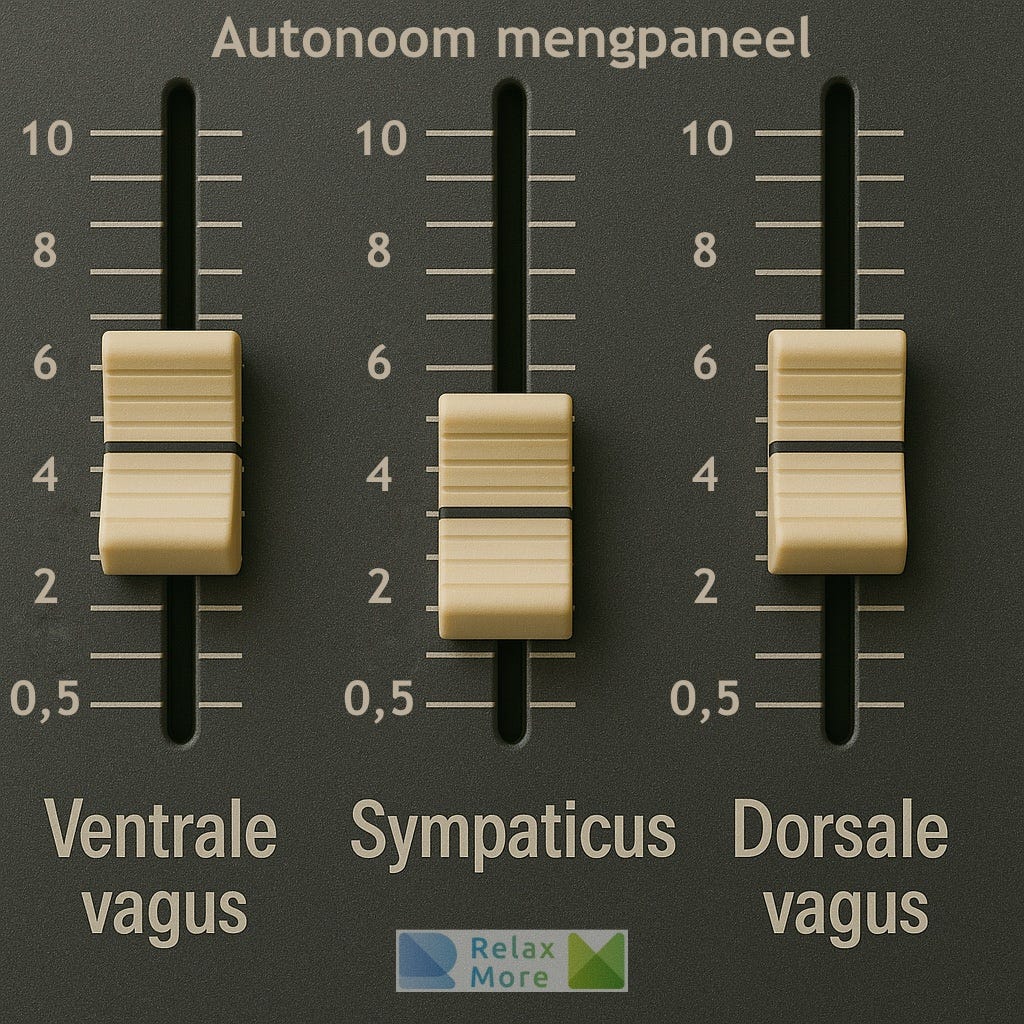
Another aspect of autonomic regulation is that the three systems do not switch on and off like light switches but shift gradually. For this reason I have moved away from the ladder metaphor and developed an autonomic mixing panel.
This yields an even more nuanced picture of how the three systems work together and allows us to name states in which two systems are simultaneously in the foreground. When you are sitting with your partner on the sofa, for example, the chances are that both your connection system and your rest-and-withdrawal system are active. Often during exercise, not only the action system is running, but the connection system is also engaged. There are countless examples of how the autonomic mixing panel might be set at any given moment.
In recent years, considerable attention has also been paid to the concepts of fawning and please-and-appease—both of which are also examples of mixed states.
In this picture, neuroception is the hand that operates the mixing panel:
Free Choice?
No one consciously chooses to enter a fight-or-flight response or to freeze. Many survivors of violence or abuse carry feelings of guilt about not having resisted or having resisted less than they feel they should have. The response to life-threatening events, however, is not a voluntary choice; our body makes that choice based on neuroception.
In polyvagal theory, there is no such thing as a bad response—there are only adaptive survival responses.
No Fixed Sequence
Which autonomic state is activated in a given situation—whether safe or threatening—and how it is expressed differs from person to person. The evolutionary hierarchy is fixed; the three systems have developed in the sequence described. But the hierarchy does not mean that you always move from the connection system to the action system; this ‘phase’ can be skipped entirely, and someone may shift directly into the rest-and-withdrawal system.
Earlier experiences can cause the connection system to be less developed or to become depleted quickly, so that even a mild threat leads someone to slide into action or withdrawal. A very severe situation may also mean that the connection system is not further activated; after all, there is no point in seeking help when your house is on fire—you need to run (action system → flight).
Structures Involved
Central to all of this is the evolution of several cranial nerves, with the vagus nerve playing the most prominent role. You can read a great deal about this same vagus nerve these days on so-called social platforms. In addition to the vagus, four other cranial nerves play a role in the polyvagal story. And from there, the whole body, the entire hormonal system, and the entire metabolism are involved.
Pillar 3: Co-Regulation—Regulating Together
Our nervous system is not a solo performer. As mammals, we are naturally oriented toward connection with others, and that connection has a direct physiological effect. The presence of a calm, safe other person literally calms our nervous system—and when we are in a calm state ourselves, we can help others calm down too. This is what we call co-regulation: the mutual influence of nervous systems on one another.
How Does Co-Regulation Work?
The ventral vagal circuit (the connection system)—the evolutionarily newest and most developed part of our autonomic nervous system—is neurally connected to the muscles of the face, voice, and head. This connection enables social communication: a soft voice, an open facial expression, gentle eye contact. Through these channels, our nervous system constantly ‘reads’ the state of the other person’s nervous system.
A calm therapist, an attentive parent, a settled friend—their regulated nervous system functions as an external regulator for ours. This is not a metaphor or poetry. It is neurobiology.
Co-Regulation in Practice
The concept of co-regulation is helpful in explaining how and why young children develop their nervous system in the context of a caregiver and why early attachment is so important.
We also know that the therapeutic relationship can itself be healing, independent of the method the therapist uses; in this sense, the therapist ‘does’ something simply by being present. Most people have experienced, at some point, how someone in crisis can be calmed simply by being fully present—and conversely, how someone in panic is not helped by a loved one who also falls into panic. In groups, the dynamic can be powerful in both directions: co-regulating as well as destabilizing.
To make optimal use of co-regulation, it is important that professionals themselves have a well-regulated autonomic nervous system and can remain regulated even when their client is not.
Co-regulation is listed here as the third pillar, but you may well understand by now that its effect becomes visible through neuroception in an autonomic state. Co-regulation could therefore also be placed first in the sequence! Polyvagal theory is describing a genuinely dynamic system.
Self-Regulation as a Complement
If you learned to co-regulate well as a child, the capacity for self-regulation develops. Techniques such as mindfulness, breathing exercises, Tai Chi, and Qigong help calm the nervous system from within.
Why Is Polyvagal Theory Important?
The theory does not only offer an explanation for what happens in the nervous system—it also has direct implications for how we relate to people, to complaints, and to recovery.
Education and Child-Rearing
A safe environment is not a luxury; it is the physiological prerequisite for learning and development. A nervous system operating in defense mode—with the connection system less active—cannot learn optimally. Children who grow up in unsafety develop a nervous system that is constantly on alert. The consequences are measurable well into adulthood, as extensively demonstrated by research into Adverse Childhood Experiences (ACE).
For the (Psycho)Therapeutic Practice
Polyvagal theory shifts the therapeutic gaze from ‘What is wrong with this person?’ to ‘What survival response has this nervous system learned?’ That is an important and less stigmatizing perspective. Body-oriented therapies such as Somatic Experiencing® work directly with autonomic state, far less through talking and cognitive processing.
For the Professional Themselves
Co-regulation makes clear that a professional does not only apply techniques, but is present with their own nervous system. A regulated professional offers a regulated space. This may well be the most active ingredient of any therapy or coaching session. As Stephen Porges said:
“Safety IS the therapy.”
Stephen Porges
For Medication and Treatment Choices
Insight into autonomic dysregulation helps explain why certain treatment methods work and others do not. It also offers entry points for new interventions—from HRV biofeedback to voice use, from group therapy to body work.
For Society
At the societal level, polyvagal theory asks: which environments create safety, and which create chronic threat? This touches on architecture, policy, healthcare, and education — everywhere that people live and work together.
For each of these points, articles will be appearing on this website in the coming period—stay tuned!
“Polyvagal Theory is for everyone interested in evolution, human development, and the workings of the social brain. I encourage you to journey with Dr. Porges, as he shares his vast knowledge of the brain, our bodies, and our interpersonal emotional connection in a way that will deepen your understanding of and appreciation for both our social and inner selves.”
Louis Cozolino, Professor of Psychology
Implications of Polyvagal Theory
When Porges published polyvagal theory in 1994, he did not yet anticipate that pioneers such as Peter Levine (founder of the body-oriented trauma therapy Somatic Experiencing®) and Bessel van der Kolk (professor of psychiatry specializing in post-traumatic stress disorders) would take such a keen interest in his work.
Porges had not yet interpreted immobilization as a defense strategy in animals as a potentially traumatic response in human beings. But his theory finally explained what Levine, Van der Kolk, Ogden, and a number of other body-oriented pioneers had known for so long: the path to trauma healing runs through the body. This is how the sense of safety can be trained and restored.
We are, and will remain, both human beings and mammals—and for our survival, we need relationships and interaction with others. These are, for many people, the most challenging areas of life, and here lie clear links with themes such as attachment, intimacy, love, and friendship.
Video?
This wonderful short film with Dutch subtitles offers a clear and accessible explanation of the entire polyvagal theory.
If you have questions after reading this article, please post them in the comments below so that others may benefit from your question too.
If you found this article worth reading and (not yet) feel like getting a paid subscription, you can always treat me to a cappuccino!